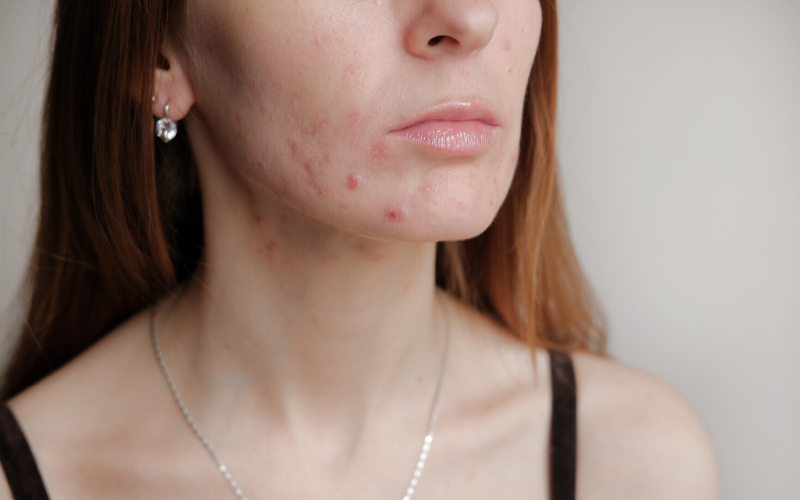
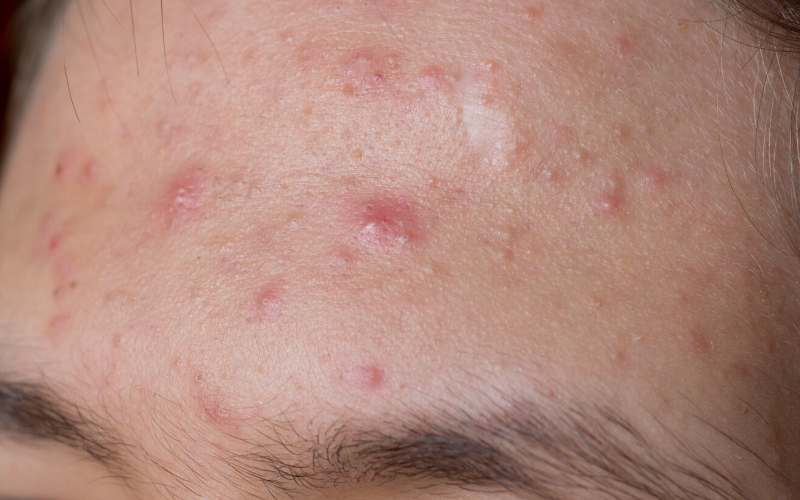
You roll out of bed, wash your face, and there it is: another dreaded pimple appearing.
You’re in the 80% of women between the ages of 11 and 30 with acne — could hormones be the culprit behind your issues?
Thankfully, there are many treatments and even dietary changes that can break the breakout cycle. As a dermatologist, I’ve seen that treating hormonal acne works best from the inside out. If your face is having more breakout success than Hamilton, there is holistic help.
What is hormonal acne?
Unsurprisingly, hormonal acne is a skin condition acne triggered by an imbalance in hormones. While hormones aren’t inherently bad — in fact, we all have them — unbalanced levels can lead to many unwanted side effects.
While it’s easy to conflate adult acne and hormonal acne, there are some specific signs that acne is caused by chemical imbalances in the body:
- Hormone-associated events: Menopause, pregnancy, menstruation, or puberty can all lead to hormonal acne
- Stress: When you’re on edge, the body produces cortisol, which affects other hormone levels.
- Breakouts on certain areas of the face: Depending on your age, you may notice consistent locations of your acne issues that signal hormones as a root cause.
We’ll unpack these indicators more thoroughly below, but if your breakouts don’t share some of these traits, you may have something else to blame than your hormonal state.
Menopause, with its elevated testosterone or androgen levels, can increase chances of hormonal acne as well. As estrogen levels dip and our hormones find a new normal, clear skin can be one of the casualties.
So, what does hormonal acne look like?
Causes & Symptoms
How do you know if you have hormonal acne? You can know if you have hormonal acne based on the placement of the zits, your hormone levels, and possibly even your age.
What causes hormonal acne? In females, hormonal acne is caused by a rise in androgen and testosterone levels, usually coupled with a drop in estrogen. This also is linked to a rise in sebum production, as oil glands are sensitive to testosterone.
These fluctuations signal to your oil glands to increase sebum production, thus making your face more oily. This sebum can clog pores and irritate skin, producing acne.
Hormonal breakouts can result from not only issues like dead skin cells clogging oil the pores, but also an overproduction of P. acnes, a bacteria that causes acne.
Inflammation occurs, from these factors or environmental triggers, leading to acne breakouts.
In most women, levels of estrogen and progesterone vary widely across the month due to the menstrual cycle — yes, it’s more than just the week of your period. These fluctuations can signal your skin to inflame, clog, and produce oil.
What are the symptoms of hormonal acne? Hormonal acne can appear as:
- T-zone acne: As a teen, hormonal acne often develops in the “t-zone,” or in a T-like shape along the forehead, nose, and chin. This is often where excess oil is produced.
- Jawline: When adults develop hormonal acne, it tends to fall along the jaw and chin.
- Cysts: Cystic acne forms deep under the skin, leaving large, inflamed, and tender bumps below the surface.
- Zits: Whiteheads, blackheads, and small pimples or bumps are likely to occur, particularly in oily parts of the face.
The process of puberty, as well as hormonal conditions like PCOS or thyroid conditions, can contribute to hormonal acne. Finally, oily skin is also more prone to these blemishes.
There are abundant myths about where acne comes from. Here are some of the truths you need to hear:
- Hormonal acne is possible long after your teen years. Women experiencing hormonal fluctuations, certain health conditions, or even menopause can struggle with this.
- This doesn’t mean you don’t wash your face frequently enough. Over-washing the face can irritate the skin and signal it to produce more sebum, the very thing you’re hoping to avoid.
- Toothpaste isn’t the answer. This remedy is an old one, but toothpaste doesn’t change oil production, and the chemicals it contains may not be kind to your skin.
While the symptoms vary slightly, hormonal acne is still possible to identify from other forms of acne based on your breakout area.
How do I get rid of hormonal acne? You can get rid of hormonal acne through topical treatments, prescriptions, diet changes, and natural remedies.
Below, you’ll find a list of what I recommend as a dermatologist for treating hormonal acne.
Topical Treatments
Topical treatments are ones that you apply directly to the face. These can include gels, creams, cleansers, and serums. However, they’re not all equally effective, so here are my top choices.
Over the Counter
These topical treatments can be purchased at many drugstores, supermarkets, online and some even at organic markets. They are easy to pick up, but sometimes may not pack the punch that a prescription topical medication would have.
If you’re wanting a topical acne treatment that’s a bit milder than prescription offerings, pick up one of the skincare products listed below.
- Tea tree oil (diluted): A study recently found that diluted tea tree essential oil significantly relieved acne in mild to moderate cases. Be sure to dilute tea tree oil with a carrier oil, so as not to further aggravate the skin.
- Salicylic acid: If you’re struggling with blackheads or whiteheads, try this acid, which may even prevent future breakouts if used regularly.
- Glycolic acid, or AHA: This chemical exfoliates the skin and dissolves the bond between dead skin cells that can clog the pores.
- Resorcinol: Resorcinol is an antibacterial compound that breaks down hardened skin.
- Benzoyl Peroxide (BPO): The American Academy of Pediatrics calls BPO the “most effective” over the counter topical acne medication for teens. It kills bacteria under the skin’s surface and removes dead skin cells and excess oil.
- Bentonite clay masks with apple cider vinegar: Mixing the powdery bentonite clay with ACV is a fun and rewarding face mask that draws out impurities, comes loaded with probiotics, and calms the skin.
Prescription
If you need something stronger, your dermatologist may be able to prescribe you a more intensive treatment. While your doctor will likely have suggestions, here are some of the options available to you:
-
- Dapsone, various strengths: This helps calm inflammation and tends not to dry out your skin. It’s one of the top go-to topical treatment options prescribed by dermatologists due to its low risk of side effects and it’s not an antibiotic.
- BPO/Clindamycin combinations, various strengths of each: This power couple kills bacteria, like P. acnes, that can cause flare-ups and can help rebalance the skin microbiome.
- Adapalene/BPO combinations, various strengths of each: Adapalene is a retinoid that slows the growth of cells, reduces inflammation, and fights pimples. You already know how effective benzoyl peroxide is.
- Erythromycin, alone or combined BPO (called Aktikpak): Erythromycin is a prescription antibiotic that fights acne-causing bacteria, however resistance can develop when it’s used by itself. BPO can complement it to peel back a fresh layer of skin.
-
- Tretinoin, various strengths and combinations: Tretinoin is prescription strength retinoid that helps with blackheads and whiteheads and may also help with some of those fine lines and discoloration when used long term.
- And lots of other topical prescription options available from your dermatologist.
Topical medications are often a first step, but some hormonal acne sufferers move onto internal prescription medications to find further relief.
Prescription Medications
Prescription medications may be able to help in more severe cases of acne. These will require a visit to your dermatologist, but can also offer extra support when topical medications simply aren’t working. Here are some of the common recommendations:
- Spironolactone: This medication can reduce production of androgens, like testosterone, which can lower hormonal acne flare-ups.
- Low-dose (anti-inflammatory not antibiotic dose) short-term use of of tetracycline derived medications such as Seysara: Seysara is a new prescription option to treat deep, cystic acne by clearing up the underlying bacteria. Low-dose doxycycline is another common short-term treatment option for inflammatory acne until topicals and lifestyle changes start improving acne. Remember to take a probiotic when you are on antibiotics no matter what the dose of the antibiotic.Birth control pills: If your hormone fluctuations are severe and affecting your face and life month after month along with other systemic medical issues, birth control pills can release a measured dose of female hormones throughout the month, regulating your hormones and menstrual cycle. This is one that I do not prescribe as suggest that patients coordinate care with their gynecologist to search for underlying gynecologic issues before determining if birth control pills are the right fit.
- Isotretinoin (or Accutane): This decreases sebum production, has anti-inflammatory properties, and is a long-used method of reducing the appearance of severe acne.
- There are also several other oral options to explore with your dermatologist if needed.
Natural Treatments/Supplements
While topical and prescription treatments can be excellent solutions, natural treatments and supplements can help provide whole-body balance while treating your acne. Here are some of my favorites:
- Probiotics, which can improve the microbiome in the gut and improve the ratio of healthy bacteria to infectious bacteria
- Omega-3s, a supplement rich in anti-inflammatory properties and hormone-regulating benefits
- DIM, which can balance estrogen levels
- Green tea extract, a natural anti-inflammatory
- Vitamin D (if you’re deficient), as this vitamin plays a role in moderating insulin, a hormone, and has anti-inflammatory properties
- Ashwagandha, an herbal antimicrobial and anti-inflammatory adaptogen supplement with many calming and whole body benefits (it may reduce acne-causing cortisol levels)
- Topical CBD oil is another excellent natural topical anti-inflammatory option for your pimple breakouts.
Dietary Triggers to Avoid
Inflammation plays a major role in hormonal acne, as well as treating skin conditions from the inside out. You’ll want to stay away from inflammatory foods, along with ones that can trigger hormone changes — like insulin, adrenaline, and more.
Here’s what to avoid:
- Dairy (including whey protein)
- Sugar
- Processed foods (particularly high glycemic ones)
- Fried foods
- Alcohol
- Gluten
- Eggs (non-organic)
- Caffeine
Eliminating these foods from your diet is a major way to help reduce hormonal swings and inflammation. Don’t let the solution stop with a topical treatment or pill — add lifestyle changes that will benefit your hormones for years to come, breakouts or not.
Acne Treatments to Avoid
While I believe strongly in natural treatments and holistic approaches, not all remedies for pimples are safe or effective. Here are some acne treatments you should steer clear of:
- High dose vitamin A supplements. These can cause liver disease and other health issues.
- Vitamin C topical serums. This vitamin is used in many skincare products, but can actually sometimes aggravate acne in some patients.
- Coconut oil. This is commonly used in many skin products as a cure-all, but can clog pores and cause acne as well when used on the face
- Scrubs. Physical exfoliants can aggravate and stimulate acne glands, causing even more sebum production. The same is usually not true for chemical exfoliants, such as AHA.
Looking to the Future…
Does hormonal acne ever go away? Yes, hormonal acne does go away when treated with the right combination of medication, lifestyle changes, and diet to balance hormones. Addressing both the zits and their root cause can balance hormone levels and decrease pimples, cysts, and blackheads.
If you are suffering from hormonal acne and topical treatments aren’t working, see your dermatologist! You’re not doomed to breakouts forever, and your newly balanced body will thank you as hormones balance to the right levels.
Sources
- Zeichner, J. A., Baldwin, H. E., Cook-Bolden, F. E., Eichenfield, L. F., Friedlander, S. F., & Rodriguez, D. A. (2017). Emerging issues in adult female acne. The Journal of clinical and aesthetic dermatology, 10(1), 37. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5300732/
- Williams, H. C., Dellavalle, R. P., & Garner, S. (2012). Acne vulgaris. The Lancet, 379(9813), 361-372. Abstract: https://pubmed.ncbi.nlm.nih.gov/21880356/
- Farrar, M. D., & Ingham, E. (2004). Acne: inflammation. Clinics in dermatology, 22(5), 380-384. Abstract: https://pubmed.ncbi.nlm.nih.gov/15556722/
- Malhi, H. K., Tu, J., Riley, T. V., Kumarasinghe, S. P., & Hammer, K. A. (2017). Tea tree oil gel for mild to moderate acne; a 12 week uncontrolled, open‐label phase II pilot study. Australasian Journal of Dermatology, 58(3), 205-210. Abstract: https://pubmed.ncbi.nlm.nih.gov/27000386/
- Tang, S. C., & Yang, J. H. (2018). Dual effects of alpha-hydroxy acids on the skin. Molecules, 23(4), 863. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6017965/
- Williams, L. B., & Haydel, S. E. (2010). Evaluation of the medicinal use of clay minerals as antibacterial agents. International geology review, 52(7-8), 745-770. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2904249/
- Piskin, S., & Uzunali, E. (2007). A review of the use of adapalene for the treatment of acne vulgaris. Therapeutics and Clinical Risk Management, 3(4), 621. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2374937/
- Ahmed Mohamed, A., Salah Ahmed, E. M., Abdel-Aziz, R. T., Eldeeb Abdallah, H. H., El-Hanafi, H., Hussein, G., … & El Borolossy, R. (2020). The impact of active vitamin D administration on the clinical outcomes of acne vulgaris. Journal of Dermatological Treatment, 1-6. Full text: https://pubmed.ncbi.nlm.nih.gov/31868550/